The following article is from Massage & Bodywork, June/July 2005, used with permission.
 |
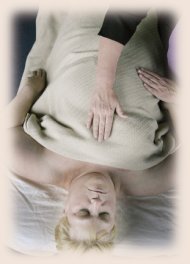 |
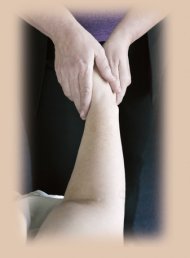
| Client
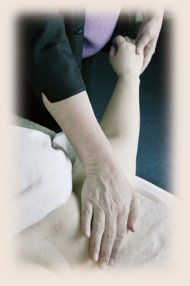
Deborah Murphy relaxes under practitioner Cheryl Johnson's touch.
Above, Johnson uses directional strokes on Murphy's
arm. Photography by Rick Giase. |
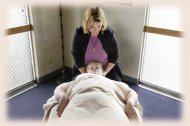 |
| Johnson, an instructor at the Colorado School of Healing Arts, has worked with Murphy through two cancer diagnoses. She says in oncology massage most any modality can and will work at given times. |
 |
 |
| Colorado practitioner Joanne James was drawn to oncology massage early on in her schooling. |
 |
 |
| Oncology practitioners say the work compels them to reevaluate their priorities. |
|
For more information |
Cancer and Human Connection
The
Making of an Oncology Massage Therapist
By Shirley Vanderbilt
Its a calling, a commitment, and a challenge, but its not for everyone. Massage for cancer clients has moved from the no-touch zone to center court, bringing with it an increasing number of compassionate, dedicated therapists. But there is a caveat to this trend. Although the bodywork profession, supported by scientific research, now provides a wealth of modalities to soothe, rehabilitate, and renew hope in those enduring the ravages of cancer, its not a matter of simply putting hands to skin.
There are dos and donts associated with performing oncology massage, especially for clients in an active disease state and those undergoing or recovering from treatment. Theres also a lot to learn about the physical and psychological challenges and changes cancer patients face in their journey. While gentle touch, such as massage to the hands or non-contact energy work, is almost always appropriate and beneficial, the needs of cancer clients will best be served by those therapists who have taken the time to become informed, instructed, and supervised in this specialized field.
Gayle MacDonald, whose book Medicine Hands: Massage Therapy for People with Cancer was a major influence in opening therapists doors and minds to oncology clients, says, With proper training, there is always a way for a practitioner to provide skilled touch to those undergoing treatment for cancer. It is wise, however, for bodyworkers to decline massaging cancer patients if they are not yet trained to do so,1 referring the client instead to a practitioner more knowledgeable in this area.
But where does one get this training? MacDonald, who also conducts oncology workshops throughout the country, has been an inspiration and guiding light for a budding cadre of instructors following in her path. Of the handful of resources available, classes range from weekend intensives to 300-hour certification programs with hands-on, supervised internship. You can get as involved as you like, but according to Kristen Will, oncology instructor for the Colorado School of Healing Arts (CSHA) in Lakewood, you cant avoid the subject.
You can go into this field for a number of reasons, Will says. It may be this will become your focus. A large group of your clients may be diagnosed with cancer. But even as a therapist with diverse clientele, she says, In this day and age, some are going to have a diagnosis of cancer and you will want to know how to treat them.
As one of the few U.S. schools offering certificate programs in oncology massage, CSHA combines class instruction with a heaping dose of internship on the front lines. Teaching Oncology Level 1, which covers the basics, is one of several hats Will wears at the school, she says. For fellow instructor Cheryl Johnson, who supervises the internship portion, oncology has become a passion, both in private practice and teaching.
The decision to pursue this path is clear for some, difficult for others. It can be not only life-changing for clients, but for therapists as well. As we take an insiders look, keep in mind this is a highly specialized field. Take from here only inspiration not liberties with the cited applications and if inspired, begin your journey with quality instruction and supervision.
The Calling
It is often a personal
cancer experience, or that of someone familiar or loved, that draws
therapists to choose this specialty. Massage therapist Cynthia Lockhart
was diagnosed with breast cancer prior to choosing massage as a career.
From the minute of diagnosis to the time I had surgery, for the first
time in my life I started having bodywork massage, reiki, healing
touch, she says. When surgery took place six weeks later, the tumor had
shrunk in size, putting Lockhart at Stage I with no spread of disease to
her lymph nodes.
She credits massage, along with some lifestyle changes, for the amazing boost to her immune system. This really made me a believer, and I wanted to be a part of that team, Lockhart says. Now, Im a very positive influence on these cancer patients who feel like their life has been taken away from them with this diagnosis. Cancer patients often feel isolated, and theres still, in this day and age, a fear. Having someone who is providing a nurturing touch for them is healing in itself. Just beginning her career, Lockhart is already involved in hospital work and says cancer patients make up half of her private practice.
Joanne James found herself being drawn to oncology from the time she decided to become a massage therapist and chose CSHA because of its certification program. Then, cancer struck her father while she was in training, and she couldnt travel to his bedside. I didnt get to work on him at all; he died within weeks, she says, further ingraining her need to work with this population. James now specializes in hospice care and is a lead therapist in a major research study titled Reducing End-of-life Symptoms through Touch (REST), being conducted at the University of Colorado School of Nursing in Denver.
In addition to having several family members diagnosed with the disease, Jan Wilson tells about working with a cancer client who was apprehensive about hair loss and wanted to keep her wig on during treatment. After Wilson explained that she, herself, had been partially scalped in an auto accident and understood what it was like to be bald, the wig came off and the client enjoyed a needed scalp massage. It really touched me, Wilson says, and the comfort level she and the client shared sparked her interest in oncology massage. Oncology certificate in hand, Wilson now combines hospital and hospice work with private practice.
Covering the Basics, Level 1
At CSHA, students
entering the oncology program are well into their 700-hour basic massage
training or have already graduated as massage therapists. The first
portion, Level 1, introduces the basics of cancer physiology and
pathology of the process; precautions for radiation, chemotherapy, and
surgery; appropriate bodywork modalities for cancer clients; and the
different stages of cancer from diagnosis, treatment, and recovery to
survivor or terminal. MacDonalds first book is a mainstay reference and
class time includes a small amount of hands-on practice.
Even though the focus is oncology, Will says the course lends itself to any hospital- or hospice-based work with the seriously ill. Whether students stop at Level 1 or go on to internship, familiarity with the subject provides a level of comfort in knowing when to treat and when to refer out. In Level 2 internship, the real hands-on work, students are exposed to the reality of the cancer patients experience at all levels of treatment. Unique to the program is the inclusion of CSHAs basic level Trauma Touch, which examines trauma more in-depth. To round out certification hours, continuing education in hydrostone, reflexology, and polarity therapy is also required.
The reason for such a lengthy training process is obvious. Cancer is a complicated disease, and each case, its treatment, and impact on the client, varies. The idea that massage can spread cancer cells is no longer an issue, MacDonald says, and gentle, conscious massage will not cause cells to become metastatic. But, many other conditions related to cancer and its treatment are of immediate concern when performing bodywork.2
For example, chemotherapy (Will says there are 50 different types) targets not only cancer cells, but can also destroy any healthy, rapidly-dividing cells. Thats why hair falls out, she says. It compromises the lining of the mouth, stomach, and intestines, causing nausea, diarrhea, and lack of appetite, which lead to fatigue. Immune system response is lowered by the impact on rapidly dividing cells in bone marrow. All of this influences the how, when, where, and why of bodywork choice for the therapist or if treatment that week is even appropriate at all.
Radiation is another area where training matters. If its external, Will says, it always has an entrance and exit site you want to be aware of both sites. Basically were avoiding that area because the skin is compromised. Therapists also need to be aware of organs the radiation is passing through. Here, working at a distance with reflexology points for those areas may be appropriate. Infection would be a whole other contraindication, she says. However, a well-trained therapist can be the eyes and ears for the nurses, reporting any signs of infection while obviously avoiding contact with the area.
In addition to physical factors, Wills course addresses emotional and psychological aspects of cancer treatment. For instance, a client in remission may still be dealing with the residual effects of chemotherapy and radiation. In fact, massage can be supportive in relieving stress, anxiety, or depression for both clients and caregivers. These are but a few of the enormously complex issues surrounding cancer care for which a therapist needs education and preparation. But just as important is the second piece of training supervised practice applying these skills on the front lines.
Into the Fire, Level 2
The internship portion
of CSHAs certification requirements provides a piece often missing in
some oncology training programs. It has a two-fold purpose: to better
prepare students and to give them an understanding of what clients go
through in all phases of their medical treatment.
Im sure its a bit of a wake up, Johnson says. Reality doesnt hit until the student is actually in the thick of it. You get there, and you cant control the situation the way you thought you would. Its moment by moment and day by day. It puts them right in the fire. Inspiration happens all across the board. Some stay some decide its not for them. Even if they choose not to specialize, there are lessons to take away.
One of those lessons is to be ready for all situations. You cant plan anything, Johnson says. Its whoever is open to massage. The patient might be too fatigued, or sleeping, or in pain. By incorporating out-patient radiation, hospital, hospice, and private practice experience, students receive a comprehensive overview despite the lack of continuity in clients.
Porter Adventist Hospital in Lakewood has partnered with CSHA since the inception of the internship class. The program has been a huge hit, says Michele Carey, director of oncology services at Porter. These physicians think the program is incredibly valid, and we receive referrals directly from them. She estimates students see an average 25 patients per week, with Johnson and others treating another 20 to 30 clients weekly. Patients obtain a consent signed by the physician and any concerns are communicated at that time. Johnson addresses questions about individual patients directly to medical staff and then conveys that information to students. Hospice work is through Hospice of St. Johns in Littleton, and students also participate in treating chemotherapy patients in private physicians offices and, to simulate private practice, bring their own clients into the school clinic.
Rounding out Level 2 work is a two-hour weekly class. It functions partially as a support group and partially as continuing, advanced education, Johnson says. Its a time for processing emotional issues, sharing journals, and discussing case-related questions. Guest speakers, including a psychologist, lecture and answer questions on subjects such as self-care, grieving, vicarious traumatization, and community resources. The goal is to ensure the students have the personal and technical support they need as they go through the internship, as well as garnering a greater awareness of the cancer experience.
Patients Perspectives
Graduates of the
oncology program note there are both highs and lows in this work, but for
clients there are only rewards. Cancer patient and massage recipient Owen
Sandrol says, There arent any emotional, physical, or spiritual
downsides to massage as compared to the pretty phenomenal downsides of
medical treatment. I think there are lessons to be learned for all
disciplines in medicine in the way Cheryl is in her profession. To me,
its that cancer is an extremely frightening word, instantly synonymous
with death. Theres a lot of emotional and spiritual confusion. While
medical specialists seem only interested in the physical aspects of his
case, Sandrol says, Johnson is like an ad hoc counselor, providing that
missing piece of caring and compassion along with physical relief.
We spend some time before massage even starts, talking about whats going on and what the effect has been physically, Sandrol says. Once massage begins, he says, the talk goes down another level the emotional and spiritual impact. I think most medical physicians in the cancer field can learn from how helpful it is to spend even a couple of minutes out of the appointment to listen to what the patient has to say about what their week has been like.
Michael Jean Halgrimson, M.D., is a gynecologist and breast cancer survivor. When she began seeing Johnson during radiation treatment, she already had endured a year of chemotherapy for a fast-growing tumor. After 12 months of treatment, youre a disease entity, she says. Its very impersonal, and you go and get poisoned and then radiated every day. Its so very dehumanizing, even though its what you have to do.
Massage made her feel human again, she says. It was a really moving experience I had not anticipated. Given a 2 percent chance of survival, Halgrimson embarked on a grueling medical regimen, determined to tolerate anything. Then, seeing Cheryl and having her just put her hands on me, I felt, ÔI really am a living being inside this body. It energized me for the other stuff I was doing. It made tolerating chemo or radiation so much easier. What she does really rescues your spirit when youre in the midst of that terrible journey you hope will end up where you want.
Whether the client wants to withdraw or talk, the massage therapist is the listener. We are not psychotherapists, Will says, so our focus is on the body and the response of the body to whats going on psychologically. Our role is to be supportive and calming and to be a very neutral person in the process. Its the same for working with caregivers or family members. My experience is that sometimes its the caregiver thats more stressed out than the patient. They are needing that neutral support person as much, if not more than, the person with the diagnosis.
For caregivers, massage can provide a respite, after which they are more able to be there for their loved one. Sandrols wife, Bonnie, agrees. Theres so much attention focused on the patient, as well it should be, but its nice to have a place where I can go and be pampered for half an hour or so. Johnson treats both husband and wife, and as Sandrol says, She has compassion for both of us.
A Full Toolbox
Johnson says the joy
of oncology massage is that any modality can and will fit at given times.
What it requires is a real thorough intake with the patient and
understanding where they are in their process. At each visit, check in
with the client and adapt the bodywork to her current condition. One day
its deep tissue, the next day its a reflexology session. A case
in point
is Johnsons work with Deborah Murphy. Diagnosed in 2003 with breast
cancer, Murphys case is complicated. Following chemotherapy, she
underwent radiation at which time she began massage treatment with
Johnson. With severe radiation burns, followed by a deadly infection,
recovery from a double mastectomy was slow.
After several months of limiting bodywork to reflexology, Johnson began some gentle circulatory massage and movement therapy. We were gearing more toward the rehab piece with the scar tissue and preparing for reconstruction. You have to deal with lymph needing to be rerouted and moved around and try to get the scar tissue to be elastic. Murphy had also started an exercise and nutrition program. Then she did a 180. She has been re-diagnosed and is going in for biopsy. Now, were changing gears. Were back to gentle, circulatory holding and reflexology which she really enjoys. To me, it all comes down to being present 100 percent.
Although Swedish massage is a standard for relaxation and improving circulation, Johnson notes there are many options available for each specific case. Subtle energy techniques reiki, polarity, jin shin jyutsu, acupressure provide gentle, noninvasive work for relaxation and energetic balancing. Lymphatic drainage therapy not only supports the immune system, but also can be used to reroute lymph for those who have lost lymph nodes. Will adds that a modified hydrostone treatment is another alternative, with the soothing and relaxing quality of warm stones providing a psychological comfort.
More invasive work, such as deep tissue, neuromuscular, and myofascial release, comes into play during the rehabilitation phase in order to work on scar tissue and chronic holding patterns. Were not physical therapists, Johnson says, but were trying to soften that tissue and basically get some strength back. At any time during the course of treatment, you can modify them so theyre very gentle.
Johnson advises her students to err on the side of caution and forego using aromatherapy while patients are in treatment. The reason is because most students of massage are not aromatherapists, she says. With only one or two days of training under their belt, theyre not equipped to understand the interactions of essential oils with chemotherapy or radiation. Its best left to the aromatherapy experts.
Therapy for the Therapist
Self-care is an
important aspect of any massage training program. If youre working with
someone who has gone through a lot of trauma, both physically and
psychologically, Will says, that takes a toll on the massage therapist
to be present in the face of that level of suffering. We focus a lot on
how we replenish ourselves so our cup is full and we can be fully present
for the clients.
Mutual support is one avenue. Another resource lies in pursuing outside interests that bring joy to life and prevent burnout. One book Ive found really helpful is Cancer as a Turning Point by Lawrence LeShan, Will says. A research and clinical psychologist, LeShans therapeutic approach emphasizes individual expression of those ways of relating and creating that inspire inner enthusiasm, which in turn stimulates the immune system. Will encourages her students to identify and pursue those passions. But each person has to put that together for themselves, she says, whether it be art, music, or something else.
To prepare students for encounters with death, Johnson includes a death meditation in Level 2, taking the group through a visualized scenario of what it would be like being on the bed, surrounded by loved ones, identifying what they believe is next, examining their lives. Its to get them to see that death is another part of life and is natural and normal, but its one of the tougher ones for them sometimes. Caregivers, and their responses during the stages of grief, are discussed, as well as the therapists experience of letting go. Students all agree it changes their perspective. This is especially true for Lockhart. Even knowing her own cancer can reoccur, she says, It has given me a completely different outlook on dying.
Hospice and Hand-holding
Working with a client
until death can be challenging, but with one long-term client, Wilson
says, the joy she received from providing comfort outweighed her sadness.
Our last session together was difficult. He was incoherent and agitated
and going in and out of consciousness. Doing the usual foot massage, which
he so loved, wasnt having its usual relaxing results, but one of the
things I did understand him say was to hold his hand. And so I did just
that, for a long time.
Although most of James experiences have been positive, she says flexibility is a must when entering someones home. Its just a fact of life that people dont change when they get cancer. Whats most difficult for me is when I see family dynamics that are not good. Somebody is dying from cancer and the spouse is in denial or angry and taking it out on the patient they never had a good relationship and now its more obvious. The family dynamics are not always overly comfortable and you do, as a massage therapist, step right into that when you come to their house.
Sometimes its not the human element, but the animals that create a less-than-perfect environment. In the home of a terminal client she treated for more than a year, James had to contend with the clients small dog climbing under the covers and barking at her while she worked and a cat that used her leg as a scratching post. Toting heavy equipment for home visits is also demanding. Its harder work. I try to limit that type of work to those clients who cannot come into the office and I charge more for that.
James points out a final, inescapable truth of hospice work. Attrition affects her business to a greater degree than therapists working with clients in remission or active treatment. Career-wise, I realize it makes it more difficult to keep a practice going because the client base is shrinking as you go along, she says. Limiting her hospice load to about 60 percent or less, she says, enables her to continue this as her major focus while maintaining a stable 40-percent base of healthy clientele. Nurturing relationships with local cancer organizations and affiliations also keeps referrals coming in.
The Human Connection
Theres an element to
oncology massage thats almost beyond words. Spiritual is how Wilson
describes it. I say that because you just know youre doing a different
kind of work. You know youre there to make them as comfortable as
possible and just be with them. Its a sense of human connectedness at its
highest. That connection, generally felt with any client, is even more
heightened and palpable with these clients. Plus, knowing they are in
their last days, I think, makes you just so much more aware of the
spiritual element of life.
Wills thoughts are similar. One benefit of going into oncology massage is it brings you face-to-face with whats important in life. There are questions anyone diagnosed with a serious illness, or has a loved one with serious illness, will have to face. She calls them The Big Three What do you feel is the meaning of life? What is your understanding of death and dying? How do you make sense of the suffering we all go through?
Looking at the questions and not running away from them makes us feel more alive and more connected with life, Will says, and its a necessity for being a massage therapist, because our clients are face-to-face with those questions. For her students, the decision of when and if they face their own fears surrounding mortality may depend on their readiness or circumstances in their lives. But if were not looking at those big questions and engaging in our own conversations with ourselves about what that means, then we cant do this work. And its not for everybody.
For more information on Colorado School of Healing Arts oncology massage certification program, call 800/233-7114, or visit https://csha.net/.
References
1 MacDonald G. Cancer,
Radiation, and Massage: The Benefits and Cautions. Massage &
Bodywork. 2001 Aug/Sept:17.
2 Ibid.,
21.
Share your thoughts! Click here to send a letter to the editor and let us know what you think. Your letter may be used in an upcoming issue of Massage & Bodywork magazine.
Please close window after reading.